
Ottawa’s Mayor and Council Are Failing on Addiction and Homelessness — Alberta Shows a Way Forward
A structured, recovery-oriented system could help Ottawa break the cycle of addiction, homelessness, and public disorder.
Ottawa’s approach to homelessness and addiction is failing. Despite hundreds of millions spent on shelters, outreach, and harm-reduction programs, visible encampments, open drug use, and mental-health crises persist across neighbourhoods such as the ByWard Market, Lowertown, and Centretown.
According to Ottawa’s 2024 Point-in-Time Count, 2,952 people are experiencing homelessness—a 78 percent increase since 2018, with 37 percent reporting substance use challenges and 42 percent reporting mental health issues, illustrating the intertwined nature of addiction, trauma, and housing instability.
The Crisis in Real Numbers
Recent Ottawa Police Service (OPS) data underscores the ongoing emergency. In 2024, OPS responded to 1,482 overdose calls and administered naloxone 128 times. By mid-August 2025, officers had already responded to 364 overdose calls and administered naloxone 29 times, saving at least 24 lives so far.
“The use of illicit substances, particularly synthetic opioids such as fentanyl, remains a major contributor to overdoses in our community,” said Staff Sergeant James McGarry of the OPS Drug Unit. He emphasized the “devastating impacts” on families and emergency services. “Encouraging open dialogue about this issue is essential. It helps raise awareness, enables those at risk to seek help, access treatment, and receive the support they need.”
These statistics, from Ottawa’s own police service, confirm the city is in the midst of a public-health and public-safety crisis.
Why Ottawa’s Current Policy Isn’t Enough
Some Ottawa councillors, including Ariel Troster, Shawn Menard, and the NDP MPP for Ottawa Centre, Catherine McKenney, have defended harm-reduction strategies such as needle exchanges, supervised consumption services, and low-barrier shelters as essential for protecting vulnerable populations.
Approaches to tackling addiction and public disorder are evolving at the provincial level. On March 13, 2026, the government of Doug Ford, Premier of Ontario, confirmed that the province will end funding for supervised consumption sites and redirect those resources toward treatment-focused programs. The province has said the move is intended to shift the system away from crisis management and toward recovery, with new Homelessness and Addiction Recovery Treatment (HART) hubs designed to connect people struggling with addiction to treatment, mental health care, and housing support. The goal is to prioritize “treatment, recovery and supports that help individuals move toward long-term stability while protecting Ontario communities.”
Concerns about the impact of existing policies have also been raised within Ottawa City Council itself. Stéphanie Plante, City Councillor for Rideau‑Vanier, which includes the ByWard Market and several frontline social-service facilities, has warned that the concentration of shelters and addiction services in the downtown core has placed immense strain on surrounding neighbourhoods. In public remarks, Plante noted that her ward now contains “12 shelters and two hotels that function like shelters,” arguing that the current approach has not produced the improvements residents were promised in terms of safety, street disorder, or visible drug use. Her comments reflect growing concern that the existing system is managing the crisis rather than solving it.
Taken together, the provincial policy shift and the concerns raised by frontline municipal leaders reinforce a broader conclusion emerging from jurisdictions that have confronted the addiction crisis more aggressively: harm-reduction services alone are not enough. Without structured pathways into detox, treatment, recovery housing, and long-term support, people often remain trapped in the cycle of addiction and homelessness. That reality is precisely what the Alberta recovery model was designed to address.
Recent research from Red Deer, Alberta, underscores this point. When a supervised overdose prevention site closed in 2025, predictions of skyrocketing deaths did not materialize. Instead, engagement with opioid agonist therapy rose 63 percent (from 9.9 percent to 16.1 percent) among former clients, demonstrating that people will choose recovery when the system actively supports it.
The Alberta Recovery Model: A Blueprint for Change
The policy debate unfolding in Ontario mirrors a broader shift occurring elsewhere in Canada. In Alberta, a recovery-oriented system that prioritizes treatment, structured housing, and long-term reintegration is already demonstrating measurable results.
Marshall Smith is the Principal Architect of the Alberta Recovery Model and a person in recovery who battled addiction and homelessness for years. Smith lived in the alleys and garbage cans of Vancouver’s Downtown East Side before getting clean and eventually becoming Chief of Staff to the Premier of Alberta. Over the past two decades, he has created residential recovery programs integrating detox, treatment, housing, employment pathways, and long-term support. His work has achieved a 40 percent reduction in fatal overdoses in Alberta.
Smith’s philosophy is straightforward: “What you live in, you learn. What you learn, you practice. What you practice, you become. What you become has consequences.” In Alberta, individuals are not just surviving—they are learning the routines, skills, and community connections needed to reclaim their lives.

ABOVE: Marshall Smith (Photo: Megan Albu)
Early intervention is central: outreach and emergency teams actively connect people on the streets to medically supervised detox programs, rather than allowing them to cycle indefinitely through shelters, parks, and emergency departments. Once stabilized, residents transition into structured treatment facilities with counselling, life-skills training, peer mentorship, and job or education support. Recovery does not end there; residents move into long-term substance-free recovery communities with ongoing support to ensure sustainable reintegration.
Alberta has committed $350 million to develop 11 recovery community facilities and associated supports. Programs like the Virtual Opioid Dependency Program offer rapid access to treatment medication with no wait lists, while coordinated navigation services guide individuals to the right level of care at the right time. This model recognizes addiction as a chronic health condition—not a lifestyle choice—and pairs housing with treatment and community reintegration support, producing better outcomes and less strain on emergency services over time.
Intervention is required: Alberta’s model demonstrates that actively removing people from streets and connecting them to structured treatment, rather than simply tolerating open drug use, achieves meaningful recovery and reduces public disorder. Ottawa can replicate this
A Path Forward for Ottawa
Imagine recovery communities where individuals live in safe, substance-free housing while learning the skills to rebuild their lives. Imagine treatment programs directly connected to job training, mentorship, and ongoing support. Imagine a city where policy doesn’t just keep people alive; it helps them thrive.
Evidence from Alberta proves this is achievable. The cost of inaction, to taxpayers, neighbourhoods, and human lives, is far higher.
Practical Policy Recommendations (Based on the Alberta Experience)
• Integrate Recovery-Oriented Care with Drug-Free Recovery Housing: Pair housing with coordinated access to substance use treatment, mental health services, and recovery supports.
• Expand Timely Addiction Treatment Access: Reduce wait times and dramatically expand recovery bed capacity to provide care when people are ready.
• Strengthen Community-Based Supports: Fund peer support programs, recovery coaching, and life-skills training.
These recommendations are rooted in the evidence-backed Alberta model, where structured recovery has improved outcomes, reduced fatalities, and lessened strain on emergency services.
Ottawa vs Alberta Recovery Model: Key Metrics Comparison
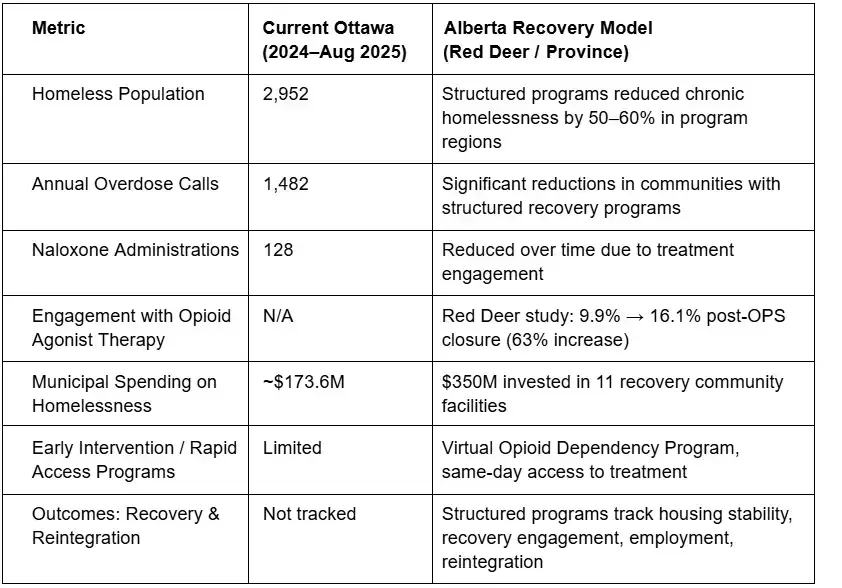
Sources: Ottawa Police Service, 2024–2025; Alberta Recovery Model data; Red Deer OPS closure study, Addiction, 2025.
Intervention Is the Way Home
Ottawa is compassionate, but compassion without structure is not enough. Every year, hundreds of millions are spent managing symptoms—emergency shelters, crisis beds, hospital visits, and policing—without addressing the root causes.
Alberta’s results demonstrate that when recovery pathways exist and are accessible, more people will take them. The Red Deer data showing a 63 percent increase in treatment uptake after the OPS closure illustrates the principle: recovery is possible, but only when the system actively supports it.
Mayor Sutcliffe and Ottawa City Council have approached this crisis with good intentions, but the data shows that Ottawa’s current approach is not breaking the cycle of addiction and homelessness and is falling short for the city, those struggling with addiction, and the broader community.
It would be wise for Council to consider the Alberta Recovery Model and explore how a structured, recovery-focused approach, with measurable success in helping people move from the streets into treatment, stable housing, and back into society, could work in Ottawa.
Ottawa can choose to endlessly manage addiction on the streets, or it can build a system that actually brings people home, into recovery, and back into society.
The Alberta model shows that the tools exist.
The question is whether or not the Mayor and Council have the will to try something different.
Header image: A collage featuring scenes from Ottawa’s ByWard Market and Lowertown.











